Sterilization often appears straightforward in theory, yet its critical importance is only truly apparent when a failure occurs. In labs, hospitals and production facilities, a single failure in the sterilization process can create problems that are difficult to reverse. Dry heat sterilization has been around for a long time and it still earns its place in modern settings for good reason.
In this guide you will learn how dry sterilization works, the principle behind it and the actual procedure in industries.
This blog gives an overview of dry heat sterilization that details its definition, instruments, principles, benefits, formulas, limitations, and factors affecting efficiency. Also, it's a comparison with some other methods and FAQs on the topic for better enlightenment.
What is Dry Heat Sterilization?
Dry heat sterilization is a process of using high temperature air to eradicate microorganisms and make instruments or surfaces sterile without any moisture. In this process, no steam and no chemicals are involved.
It is one of the oldest sterilization methods still in active use and it has stayed relevant because it handles materials that moisture based methods simply cannot. Glassware, metal instruments, oils, powders — things that would be damaged or altered by steam get processed cleanly with dry heat. No residue is left behind either which matters in a lot of settings.
It involves the application of high temperatures to materials to sterilize. The principal mechanism involved is thermal decomposition whereby the proteins and enzymes of the microorganisms get denatured and consequently killed by structural disintegration. Since this process doesn't involve moisture, it is quite appropriate for the application in cases of those items that are heat-stable but moisture-sensitive, just like autoclaving (steam sterilization). This method does not need moisture, thus is suitable for those items that are heat stable but moisture sensitive just like autoclaving or steam sterilization.
The range of temperatures between 160-180°C (320-356°F) should be applied in dry heat sterilization. The possible exposure time varies from about 1 to 2 hours, depending on whether the material is to withstand slight or high sterility degradation. Dry heat sterilizations prefer all materials that are prone to degradation or corrosion when it comes to steam or another moist heat method. For instance, glass, metallic, powders, or oils.
Instrument used in dry heat sterilization
The device used to achieve dry heat sterilization is referred to as the dry heat sterilizer, or dry heat oven. Dry sterilizers are devices that rely on high temperatures to destroy, thereby making materials sterile by eliminating microorganisms through heat in dry conditions. They are used to perform the sterilization of glassware, metal equipment, powders, and other certain chemicals that can be damaged during the process due to wet conditions.

Principles of Dry Heat Sterilization
Dry heat sterilization destroys microorganisms through oxidation. Sustained heat breaks down cellular components, denatures proteins, and eventually kills the microbial cell completely.
Because there is no moisture to help conduct heat into the material, the process needs higher temperatures and longer exposure times than steam based methods. It is a slow, penetrating effect rather than a fast kill. That is not a weakness instead it is just how the method works, and understanding that helps in using it correctly.
Three things drive the outcome. Temperature, time, and how evenly heat moves through the load. If any one of those is off, the cycle cannot be relied on.
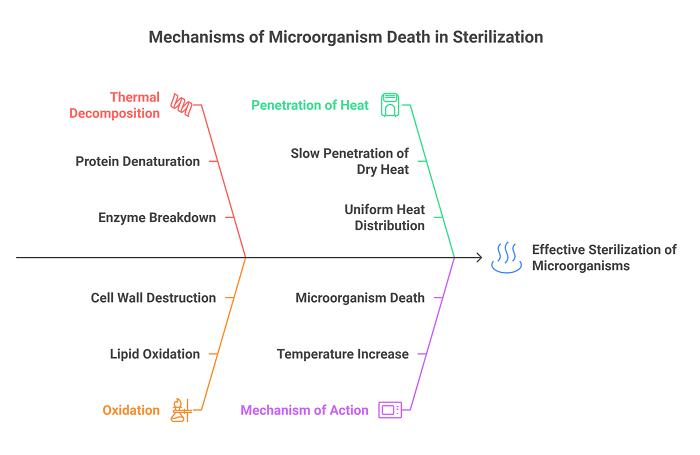
- Thermal Decomposition: Sterilizer heat breaks down the proteins and enzymes in microorganisms. This denaturation leads to a permanent loss of their biological function that kills the microorganism.
- Oxidation: Lipids will oxidize as dry heat, and walls of the cells of microorganisms, which will tear up their structural integrity and make microorganisms die.
- Penetration of Heat: It has full penetration of heat on items being sterilized so proper sterilization occurs. Dry heat penetrates slower than steam, and it will distribute the heat in the chamber so uniformly for the results' uniformity.
- Mechanism of Action: In dry heat, heat passes through the material under sterilization to increase the temperature to kill the microorganisms present, such as bacteria, viruses, fungi, and spores.
Procedure of Dry Heat Sterilization
Preparation of Materials
Every item going into the sterilizer needs to be clean and fully dry beforehand. Leftover moisture on instruments can interfere with the process and compromise the result.
Glassware typically gets wrapped in aluminum foil or kraft paper. Metal tools go into trays that allow air to move around them. Powders and oils need to be spread in shallow layers so heat can actually reach through. Overloading the chamber is probably the most common mistake, and it almost always creates uneven sterilization across the batch.
Loading the Equipment
Items need space between them for hot air to circulate. Packing things in tightly might look efficient but it blocks airflow and creates spots in the chamber that never reach the right temperature.
Nothing should be pressing against the chamber walls either. The whole process depends on even heat distribution, and anything disrupting airflow works against that directly.
Setting Temperature and Time
Standard parameters in most settings run at 160 degrees Celsius for 2 hours, 170 degrees Celsius for 1 hour or 180 degrees Celsius for 30 minutes when a faster cycle is needed.
These numbers exist for a reason. They reflect what is actually required to achieve a sterility assurance level worth trusting. Running slightly under temperature or pulling items out early is not a minor deviation. The cycle has failed at that point.
Cooling and Unloading
After the cycle finishes, the chamber has to cool before anything comes out. Hot glassware pulled into cooler air too quickly is a reliable way to get cracking or thermal shock.
Natural cooling inside the chamber is the right approach. Once cooled properly, items are sterile and need to be handled and stored in a way that keeps them that way.
Applications of Dry Heat Sterilization
Laboratory Glassware
Standard lab glassware like beakers, flasks, petri dishes and pipettes goes through dry heat sterilization routinely. Glass tolerates high temperatures without issue and dry heat leaves no residue that could affect experimental work.
Moisture based methods can sometimes leave traces or interact with certain glass surfaces in ways that are not ideal for sensitive lab applications. Dry heat sidesteps all of that.
Metal Surgical Instruments
Scalpels, forceps, and other sharp metal instruments that do not do well with repeated steam exposure are better suited to dry heat. Corrosion and edge degradation are real concerns with moist heat over time.
Dry heat preserves cutting edges far better across repeated cycles, which matters in surgical settings where instrument condition is not something to compromise on.
Powders and Oils
Pharmaceutical powders like talc, zinc oxide, and sulfur cannot go through steam sterilization. Water would change their physical properties entirely. Dry heat handles them without interference.
Oils and waxes sit in the same category. They repel moisture, so moist heat simply has no effect on them. For these materials, dry heat is not just a preference but it is the only thermal option that actually works.
Pharmaceutical Manufacturing
Glass vials, ampoules, production equipment, and certain raw materials in pharmaceutical environments all pass through dry heat sterilization. Many of these items also need depyrogenation alongside sterilization, and dry heat at the right temperature takes care of both in a single cycle.
Regulatory validation requirements in pharma are strict, and dry heat fits into those frameworks cleanly.
Microbiology and Research Labs
Research environments dealing with cultures, specimens, and precision instruments rely on dry heat because it is controlled and does not introduce outside variables. For experimental work where contamination or residue could affect results, that matters more than people sometimes realize.
How Testronix Hot Air Oven Helps in Dry Heat Sterilization
The equipment running those sterilization cycles should be reliable for accurate results. This is where the hot air oven selection actually makes a difference. Testronix Instruments manufactures hot air ovens built around consistent, uniform heat distribution throughout the chamber. Temperature stays stable across the entire cycle which is what determines whether the outcome can actually be trusted.
For labs, pharma units, or production floors where sterilization runs regularly, equipment that performs the same way every single time is not optional. It is the baseline requirement.
Their ovens are built for real working conditions, not just controlled demos. Reliable temperature control, even air circulation, and straightforward daily operation make them practical for facilities that run sterilization as a routine part of their process. If dry heat sterilization is a regular part of your workflow, Testronix is worth looking into.
Advantages of Dry Heat Sterilization
No Moisture Damage: Dry heat sterilization best suits materials sensitive to moisture including various metals like surgical instruments as well as powders or oils.
Long Shelf Life: Since dry heat sterilization can easily preserve the quality of those materials that might degrade in steam or moist heat, items sterilized this way often have a much longer shelf life.
No Rusting: Unlike moist and steam sterilization where one is likely to develop rust and corrosion on most metals, dry heat does not introduce moisture. Thus, the longevity of metal instruments remains intact.
Inexpensive: The dry heat sterilization method would also be economically beneficial since nothing except the sterilization device would be required. Effective Microbial Destruction: Dry heat Sterilization annihilates many microorganisms (typically bacteria, viruses, and fungi spores).
Factors Affecting Dry Heat Sterilization Efficiency
- Temperature and Time: The higher the temperature, the shorter the time, and the better sterilized. However, a balance has to be set for the parameters not to harm delicate materials.

- Air Circulation: Adequate air circulation must occur for uniform heating to take place throughout the sterilization chamber. Without proper airflow, unequal heating may occur along with an inconsistency in sterilization.
- Load Size and Material Type: The size and weight of the materials to be sterilized determine the necessary time and temperature for a particular sterilization process. For example, larger items or denser materials are required to be exposed longer to be properly sterilized.
Dry Heat Sterilization vs. Other Methods
Dry heat sterilization is not the most suitable option for all types of materials. Significant differences are observed in the comparison of dry heat sterilization with other sterilization methods like autoclave, ethylene oxide, and radiation sterilization.
Autoclaving: The ideal method of sterilization for the majority of items is steam sterilization (Autoclaving) because it uses moist heat but might destroy heat-sensitive materials or corrode the metals. The dry heat sterilization process is preferred when moisture is adverse.
Ethylene Oxide Sterilization: The process here requires the use of a gas for the process. However, because the gas is toxic, long exposure times and careful handling are required.
Radiation sterilization: This is practicable for only a few medical devices and pharmaceuticals but it is relatively expensive as well as highly technological equipment.
Limitations of Dry Heat Sterilization
Longer Process: Typically, it is slower in comparison to the wet methods of sterilization and consumes processing time and energy as well.
High Energy Consumption: It consumes high amounts of energy and requires high temperatures over more extended periods.
Fewer Materials Compatibility: Dry heat methods are not applicable on items that are heat-sensitive like plastics, rubber, or a particular type of electronics.
Metrics and Formula for Dry Heat Sterilization
The F0 is the value used to evaluate the efficiency of dry heat sterilization, a formula or measure to consider both time and temperature for its process. This formula is:
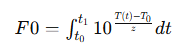
Where:
- T(t) is the temperature at a given time.
- T0 is the reference temperature (usually 121°C for moist heat sterilization).
- z is the temperature coefficient, which represents the temperature sensitivity of the microorganism being targeted.
- t0 and t1 represent the period over which the sterilization occurs.
Conclusion
Dry heat sterilization is not complicated to understand but it does demand precision to execute properly. Temperature, time, load arrangement, and equipment all have to line up for the process to hold up.
It has kept its place in labs, hospitals, and manufacturing because it genuinely works where moisture based methods fall short. For materials that cannot handle steam or chemical residues, it remains one of the most dependable options available. Knowing how it actually works makes it a lot easier to use it the right way.